Takotsubo cardiomyopathy (TCM) is known as “The broken heart syndrome” which causes sudden left ventricular dysfunction and mimics acute coronary syndromes. TCM is a significant, yet often forgotten, differential of myocardial injury and may prove to be of significant importance in the current COVID-19 pandemic. This report describes TCM as a non-COVID-19 manifestation of COVID-19.
CASE STUDY
On 7 April 2020, 10 days after the national lockdown for COVID-19 had begun, a 58-year-old previously healthy female was hospitalised for acute chest pain. She described an acute, severe, non-radiating central chest pain, starting 1 h after a verbal altercation with her employee regarding salary cuts because of the COVID-19 pandemic lockdown. There were no other associated symptoms.
The electrocardiogram (ECG) (Figure 1) recorded at home by the paramedics depicted significant ST elevation >1 mm in the precordial and lateral leads with reciprocal changes (ST depression >1 mm) in the inferior leads, features in keeping with hyperacute anterior myocardial infarction. Aspirin (300 mg) was given on site, and a subsequent ECG at the emergency department showed some resolution of the ST segment elevation in the chest leads as compared to the original ECG. Urgent coronary angiogram demonstrated normal coronary anatomy. Left ventriculography (Figure 2) showed apical left ventricular dilatation with a hyper contractile basal segment which is classical finding of TCM. A nasopharyngeal swab for SARS-CoV-2 was negative.
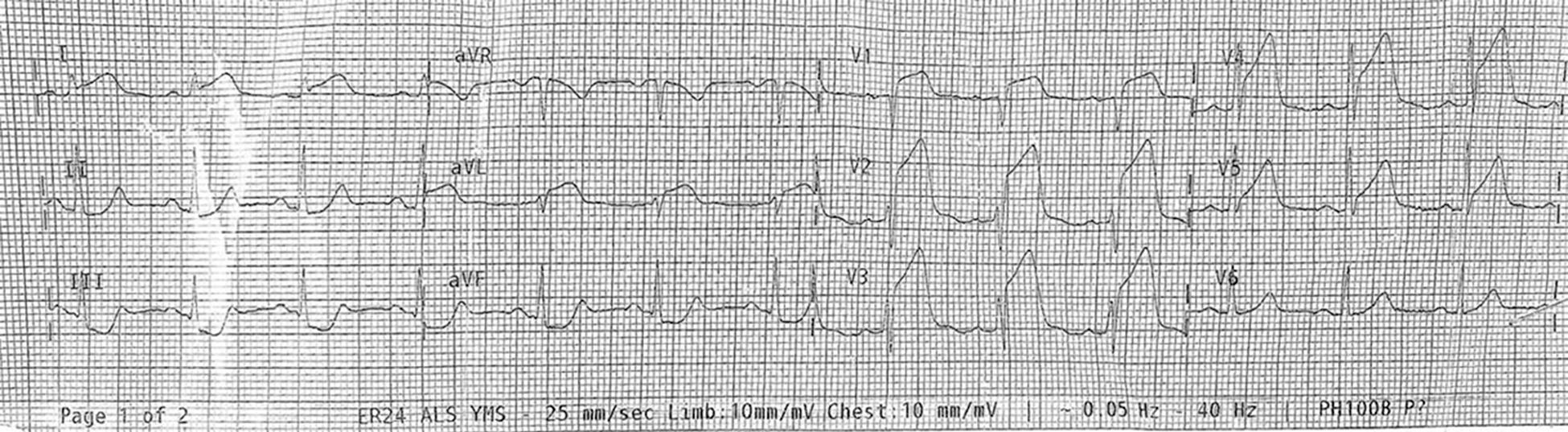
12 lead ECG demonstrating acute ST elevation in the anterior leads with reciprocal ST depression inferiorly.
On day 2, the patient developed heart failure. Anti-heart failure, anti-remodelling and anticoagulants were prescribed and the patient improved and was discharged on day 4.
On day 10 follow-up, a repeat echocardiogram showed complete resolution of the left ventricular dilatation with normal systolic function.
DISCUSSION
TCM is a transient wall motion abnormality of the left ventricular apex which is most commonly precipitated by emotional or physical stress.(1) Although a novel concept, first described by a Japanese cardiovascular specialist in 1990, it is recognised as a disease under the class of acquired cardiomyopathies.(2) TCM accounts for 2% of those with suspected acute coronary syndrome, of which 90% are postmenopausal women with an average age of 68 years.(3)
Diagnosis of TCM remains controversial; however, the most widely used diagnostic criteria are those of the International Expert Consensus Document on Takotsubo Cardiomyopathy.(4)
The pathophysiology of TCM is unknown, but numerous hypotheses exist; the most supported being microvascular dysfunction and catecholamine-induced cardiotoxicity.(1–3)
Three risk factors for TCM have been described: lack of oestrogen, inducers of emotional and physical stress and genetic factors.(1) Treatment of TCM in the acute phase is mainly symptomatic. During the ventricular recovery phase, anti-remodelling and anticoagulants are prescribed until left ventricular systolic function improves.(1,3,4)
Prognosis of TCM is reasonably favourable, with an in-hospital mortality of only 1–2% and 96% of patients recovering fully.(1,3,4)
Although case reports of TCM directly caused by COVID-19 have been described,(5) our case exhibits an indirect effect of the COVID-19 pandemic. Jabri et al. demonstrated an increased incidence of TCM during the COVID pandemic (incidence proportion, 7.8%) compared with pre-pandemic period (incidence proportion range, 1.5–1.8%).(6) Notably, all patients with TCM in the COVID pandemic tested negative for SARS-CoV-2. The immense financial, emotional, and social stress as a result of the COVID-19 pandemic are precipitants of TCM.
TCM has become a more common cardiac occurrence during the pandemic, and we believe clinicians should be more cognizant of its manifestations.


