INTRODUCTION
Cholera is a fatal diarrheal disease caused by Vibrio cholerae (a comma shaped toxigenic bacterium), primarily serogroups O1 and O139. This disease is characterized by extreme dehydration due to sever watery diarrhea; affects both children and adults; and can cause death within hours if untreated [1,2]. Cholera can be acquired through consumption of water or food contaminated with V. cholerae. In addition, V. cholerae has been associated with riverine and sea dwelling organisms, including shellfish, algae, chironomids, fish, waterfowl and amebae; these host vectors transmit cholera to humans, thus establishing the disease as a zoonosis [3]. Cholera outbreaks and transmission are associated with conflicts and accidental floods, which may lead to overcrowding of displaced people, and result in contamination of water and food [3].
Seven major cholera pandemics have occurred since the beginning of the first pandemic in 1817, and cholera is now endemic in many countries [4]. The most recent seventh cholera pandemic started in Indonesia (Asia) in 1961, and reached Africa in 1971 and the Americas in 1991 [5]. This pandemic has persisted and is currently officially recognized as an ongoing pandemic in many developing African and southern Asian countries in which cholera is endemic. A total of 1.3 billion people are at risk (primarily in Nigeria, China, India, Ethiopia and Bangladesh) of cholera, which causes approximately 1.3 to 4 million human cases and 21,000 to 143,000 deaths each year [6,7]. Although cholera has dramatically decreased in developed countries, owing to strict water sanitation and environmental hygiene measures, it remains a major scourge in many developing African and Asian countries; cholera has caused recurrent outbreaks associated with a lack of safe drinking water, climate change, population growth, poor hygiene and sanitation, displacement because of conflicts and persisting poverty [8]. Changes in environmental parameters can also influence the epidemiology V. cholerae [9]. For example, approximately 97% of cholera cases recorded between 2010 and 2021 were in countries with the lowest levels of water and sanitation services, and children were highly affected [10].
According to the multi-country cholera outbreak situation reports of 2022 and 2023 from the World Health Organization (WHO), an outbreak of cholera with high case numbers and global geographical distribution has increased mainly in Africa and the Eastern Mediterranean. The number of countries with outbreak reports increased from 23 in 2021 to 29 in 2022. The average case fatality ratio was 1.9% (with 2.9% in Africa), a value higher than that in previous years. From February 2023, approximately 25 countries (>60% in Africa, particularly eastern, central, western and southeastern Africa) continued to report cholera cases; the number may increase in the coming months, and preliminary data suggest that similar trends are expected for 2022 and 2023 [8].
The WHO and other partners at the global, regional and country levels, beyond assessing the risk of the infection at global level, have strongly supported member states in immediate response activities, such as coordination; surveillance; vaccination; infection prevention and control; risk communication and community engagement; water, sanitation, and hygiene; and operational support and logistics. However, the response capacity to the multiple outbreaks is insufficient, owing to a global lack of resources, cholera vaccine shortages, other health emergencies, and high workloads of medical and/or public health experts during multiple disease outbreaks and health emergencies; therefore, the involvement of all stakeholders is crucial [11].
In this rapid review, the current and/or ongoing cholera outbreak situation and the response to the pandemic (with particular emphasis on African regions) are discussed. The urgent need for commitment of multiple stakeholders in many nations is also highlighted. This article provides alert information to all stakeholders regarding the current expansion of cholera infection and is aimed at increasing awareness, coordinated efforts among stakeholders and the commitment of political leaders to combat the pandemic. The rapid review method was used, with an emphasis on available and recent global information found in Google Scholar, PubMed and data publicly available on websites. This review article provides current alert information regarding the high spread and upsurge characteristics of the ongoing cholera outbreak.
HISTORY OF CHOLERA OUTBREAKS
The history of cholera infection dates to the first quarter of the 19th century and continues to have major public health importance worldwide. Seven major cholera pandemics have occurred, killing millions of people worldwide [4,7]. The first cholera pandemic (1817–1821), known as Asiatic cholera, originated in 1817 in the city of Calcutta, India, and spread to and/or affected almost all Asian countries (as a result of colonization), thus causing many human deaths [12]. The second and third cholera pandemics (which are affecting most European countries, China and America) were occurred from 1829 to 1851 and 1852 to 1860 respectively. The fourth pandemic (1863–1875) began in the Bengal region and spread throughout the Middle East. The fifth cholera pandemic (1881–1896) again originated in India and reached Europe. The sixth pandemic (1899–1923), which started at the beginning of the 20th century, killed more than 800,000 people in India and spread to Eastern Europe, the Middle East and North Africa [13].
The seventh cholera pandemic (which is now endemic in many countries) started in Indonesia (Asia) in 1961, then reached Africa in 1971 and the Americas in 1991. This pandemic has persisted and is currently officially recognized as an ongoing pandemic in many endemic countries. A total of 1.3 billion people are at risk (primarily in Nigeria, China, India, Ethiopia and Bangladesh), and cholera causes approximately 1.3 to 4 million cases and 21,000 to 143,000 deaths every year [6,7].
Cholera is caused primarily by toxin producing strains of V. cholerae serogroup of O1, biotype El Tor, and O139 Bengal, which are motile, comma shaped, gram negative and single polar flagellum bacteria. Epidemiologically, cholera transmission is associated with contaminated water, environmental sanitation, and vulnerable communities (affected by natural disasters, famine, or displacement because of war, local conflict or floods); the areas typically at risk include urban and peri-urban areas, overcrowded refugee camps and remote rural locations where sanitation and clean water are limited [14]. The mode of transmission for cholera infection is the fecal-oral route, in which infection spreads through a population when feces containing bacteria contaminate water, which is ingested by individuals. After people are infected with cholera bacteria, they may recover and contaminate the water supply, thereby exposing other people to the contaminated water, who in turn become infected (Fig 1). Transmission can also occur through food washed or cooked with contaminated water [15].
Because cholera is characterized by extensive fluid loss through diarrhea, a common life-threatening complication is severe volume depletion, which leads to hypovolemic shock and metabolic acidosis [16]. According to several studies, oral rehydration therapy, antibiotic treatment and oral vaccines have saved millions of lives. Therefore, the primary treatment for cholera is the use of oral rehydration salts and antibiotics [17]. Cholera is a treatable and easily preventable disease. Apart from water sanitation and hygiene improvement, critical strategies to prevent cholera include early detection and rapid responses to contain outbreaks; a multi-sectorial or One Health approach; and coordination of technical support, advocacy, resource mobilization and partnership at the global, regional, national and local levels [10].
GLOBAL SITUATION OF THE ONGOING CHOLERA OUTBREAKS
Occurrence and epidemiology
Starting in mid-2021, the world has faced an upsurge of the seventh cholera pandemic, which is characterized by multiple outbreaks and substantial spread through previously cholera-free areas. Currently, the outbreak is occurring in many endemic developing countries, particularly in Africa and Asia. The WHO officially declared this disease pandemic an ongoing emergency. The current cholera outbreak represents the resurgence of the ongoing seventh cholera pandemic, which began in 1961 in Indonesia. The trends in cholera outbreak reports indicated that 23, 30 and 25 countries across affected regions reported cholera in 2021, 2022 and 2023, respectively [18].
As of February 2023, approximately 25 countries have reported cholera cases, and Africa and South Asia were substantially affected. More than 14 African countries (including Nigeria, Cameroon, Democratic Republic of Congo, South Sudan, Somalia, Ethiopia, Kenya, Tanzania, Zambia, Malawi, Mozambique, Zimbabwe, South Africa and Eswatini) have reported cholera cases since the beginning of 2023 (Fig 2), and new geographic areas have been affected. Other countries in Asia, the Americas, the Mediterranean and the Pacific have also reported cases. As of August 2023, 547,626 confirmed cases and 4,927 total deaths were recorded, and the number may increase in the coming months [11,19].
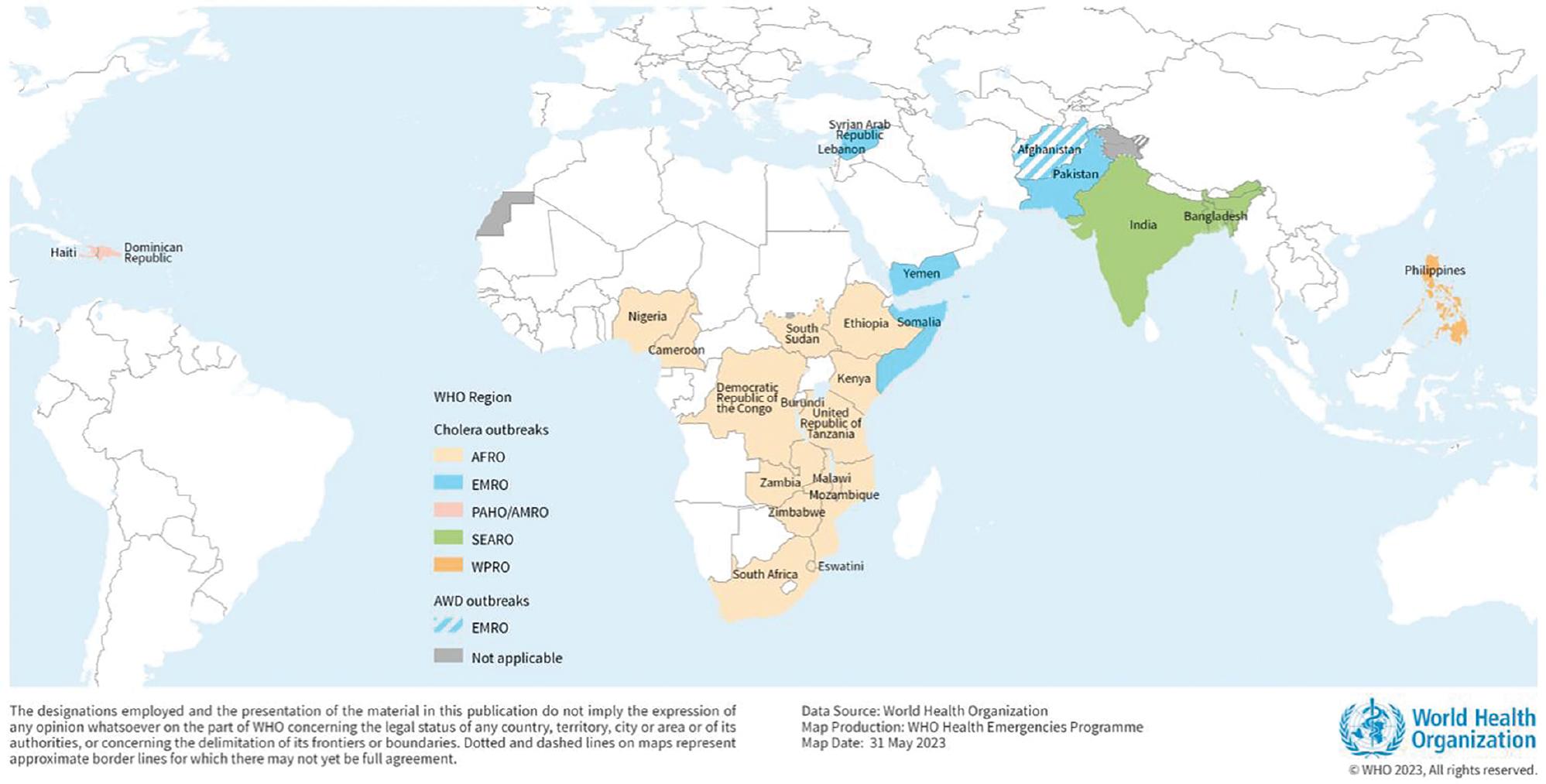
Global situation of epidemics of cholera and acute watery diarrhea reported in 2023, as of May 15, 2023 [11].
Response activities to the cholera outbreaks
Measures against cholera outbreaks in the seventh pandemic have been encouraged since the last three years of 2010s, after the launch of the Global Task Force on Cholera Control in October 2017 (a Global Road Map to 2030 with the objective of decreasing death due to cholera by 90% worldwide and eliminating the disease in at least in 20 countries by 2030). The road map focuses on multi-sectoral intervention to enhance coordination of early detection and rapid response efforts to contain outbreaks and prevent cholera recurrence in hotspots. In addition, the road map emphasizes effective technical support, capacity building, research, advocacy, resource mobilization, monitoring and evaluation. The Global Task Force on Cholera Control has worked toward cholera control, using cholera as one of poverty of indicators and an indicator of poverty, by linking the objectives of the road map to the Sustainable Development Goals [20]. Moreover, beyond assessing the risk of infection at the global level and declaring the cholera upsurge a global health emergency, the WHO and other organizations at the global, regional and country levels have extensively supported member states in immediate response activities such as coordination; surveillance; vaccination; infection prevention and control; risk communication and community engagement; water sanitation; hygiene; and operational support and logistics. Although their national response capacity has been restricted because of priority emergency issues and resource limitations, affected countries have made efforts to combat cholera since the beginning of the outbreaks. However, the general response capacity to the multiple outbreaks has been unsatisfactory because of a lack of global resources, cholera vaccine shortages, other health emergencies, the high workload of medical and/or public health experts, and the occurrence of multiple disease outbreaks and health emergencies. Generally, the current cholera outbreaks have been exacerbated by climatic effects, natural disasters, quality of reporting, lack of supplies, inadequate preventive campaigns, weak emergency responses, a lack of experienced staff, and the need for urgent and well-organized involvement of all stakeholders [11].
WHY CHOLERA THREATENS AFRICA
Sub-Saharan Africa has reported more cholera cases and deaths than any other region starting from the late 1990s [21]. The current ongoing cholera outbreak has occurred largely on the African continent, particularly sub-Saharan regions. More than 14 African countries (including Nigeria, Cameroon, Democratic Republic of Congo, South Sudan, Somalia, Ethiopia, Kenya, Tanzania, Zambia, Malawi, Mozambique, Zimbabwe, South Africa, Eswatini and Burundi) have reported cholera cases since the beginning of 2023 (Table 1), and new geographic areas have been affected (Fig 1). As of August 2023 (WHO situation report), approximately 33.68% of cases (184,474) and 64.2% deaths (3,165) were recorded in African countries [19]. In addition, the highest case fatality (3.5%) and deaths (1,761) were recorded in South Africa and Malawi, respectively. These numbers may increase in the coming months, given that heavy rain and flooding may occur in West Africa, where the rainy season is between May and October [11].
Cholera cases and deaths in Africa, as of July 15, 2023 [19].
| Country | Number of cases | Total deaths | Cases per 100,000 | Case fatality rate |
|---|---|---|---|---|
| Burundi | 581 | 9 | 4 | 1.5 |
| Cameroon | 19,395 | 463 | 70 | 2.4 |
| Democratic Republic Congo | 28,043 | 196 | 30 | <1 |
| Eswatini | 2 | 0 | < 1 | 0 |
| Ethiopia | 13,118 | 172 | 12 | 1.3 |
| Kenya | 11,835 | 194 | 23 | 1.6 |
| Malawi | 58,941 | 1,766 | 295 | 3 |
| Mozambique | 33,344 | 141 | 104 | <1 |
| Nigeria | 2,052 | 55 | 1 | 2.7 |
| South Africa | 1,274 | 44 | 2 | 3.5 |
| South Sudan | 348 | 1 | 2 | <1 |
| United Republic of Tanzania | 284 | 1 | < 1 | <1 |
| Zambia | 757 | 14 | 4 | 1.8 |
| Zimbabwe | 3,567 | 79 | 20 | 2.2 |
| Somalia | 10,933 | 30 | 89 | < 1 |
| Total | 184,474 | 3,165 | - | - |
Because developing countries are prone to predisposing factors for cholera epidemics (such as insufficient safe drinking water, climate change and severe drought, population growth, poor hygiene and sanitation, displacement of people because of war and/or local conflicts, multiple disease outbreaks, shortage of medical commodities, high cross-border movement, persisting poverty, weak infrastructure and limited resources), African countries are greatly affected by cholera and other foodborne diseases [22,23]. Therefore, the current ongoing cholera pandemic is the threat to Africa.
CONCLUSION AND RECOMMENDATIONS
Since mid-2021, a cholera outbreak has affected multiple developing countries in Africa, Asia and Oceania. As of August 2023, 547,626 confirmed cases and 4,927 total deaths were recorded, and the number may increase in the coming months. The WHO has already officially declared the ongoing pandemic an emergency. The current multi-country cholera outbreak has spread primarily in Africa, which has high numbers of cases, and new affected geographical areas and case fatality rate reports. As of February 2023, approximately 25 countries (>60% in sub-Saharan Africa) continued to report cholera cases, and the number may increase in the coming months. International and regional organizations, together with national and local administrations, have made extensive efforts in the immediate response, as well as other prevention and control activities. However, the response capacity to these multiple outbreaks is insufficient. Although affected countries have attempted to address the outbreaks since their onset, the general response capacity to the outbreaks is unsatisfactory, because of insufficient resources, cholera vaccine shortages, other health emergencies, high workloads among medical and/or public health experts, and the occurrence of multiple disease outbreaks and health emergencies. Moreover, the current cholera outbreaks has been exacerbated (particularly in African countries) by climatic effects and/or natural disasters, low quality of reporting, a lack of supplies, inadequate preventive campaigns and weak emergency responses among affected nations. Therefore, collaboration among multiple stakeholders, advocacy and extensive community awareness, regular risk assessment and information sharing, strong cross-border surveillance, sufficient resource mobilization, and very high leadership commitment and integration among all African nations are crucial to fight against the current pandemic. Combating cholera now, on the basis of the One Health approach, should be a priority among African nations.



