INTRODUCTION
Monkeypox (MPX) is a typical zoonosis that is caused by the monkeypox virus (MPXV) of the Orthopoxvirus genus, which includes the well-known smallpox, vaccinia, and cowpox viruses. Similar to smallpox virus, MPXV infection has a clinical onset with fevers, myalgias, fatigue, and headaches, which are frequently followed by skin lesions with pustular papules and ulcerations [1]. Generally, lymphadenopathy differentiates MPXV infections from smallpox virus infections. MPXV was initially identified and endemic in Central and West Africa countries, where the natural hosts are rodents and non-human primates [2,3]. For decades, human MPX cases were mostly restricted to zoonotic infections with limited human-to-human spread. Since the first confirmed MPX case on 7 May 2022 in the United Kingdom [4], >78,000 confirmed cases have been reported in more than 110 countries, including China, as of 8 November 2022 (WHO). The Food and Drug Administration (FDA) has approved two vaccines and three antiviral drugs to prevent and treat MPX, none of which are available in China.
The sudden increase in number of MPX cases and geographic expansion were accompanied by some unusual clinical outcomes and transmission routes. The number of MPX infections rapidly increased, suggesting a more effective human-to-human transmission than previously recorded. The case-fatality rate (0.025%) of the current outbreak, however, is much lower than classic MPX (1%-15%) prior to 2022 [1]. Notably, the majority of the reported cases are identified in men who have sex with men (MSM), and the rapid spread of MPX in MSM has been attributed to sexual promiscuity of affected individuals [5]. Contact with infectious viral material from skin lesions occurring during sexual intercourse has been identified as the main risk factor [6,7]. Additionally, during the present outbreak, some MPX patients had asymptomatic infections or milder symptoms with fewer skin lesions, implying the current MPXV was cryptically transmitted in populations for a long time [8]. In addition, other changes might be responsible for the novel features of this epidemic.
MONKEYPOX VIRUS MUTATIONS
Viral adaptive mutations have been reported to contribute to the initiation of the pandemic, as well as enhanced phenotypes in pathogenicity and transmissibility [9,10]. Direct comparison of historical and contemporary MPXV strain genomes are hoped to provide clues to these unanswered questions. The MPXV genome consists of a large double-stranded DNA, encoding approximately 190 genes. Before the 2022 outbreak, MPXV was classified into two clades: the Congo Basin Clade (clade 1), which is predominant in Central Africa with severe symptoms and a higher mortality rate (>10%), and clade 2, which circulates in West Africa with milder cases and a lower mortality rate (1%-3%). The rapid transmission of MPXV might be related to the genomic divergence from these two clades. Recently, Gomes and colleagues [11] analyzed the phylogenomic characterization of the first viral genome sequences of the 2022 MPXV outbreak. Gomes et al. [11] suggested that the current outbreak clustered with 2018–2019 cases (clade 2) linked to an endemic country, indicating that the current global outbreak originated from a single epidemic region. The current lineage, however, is segregated to a different phylogenetic branch (B.1) with approximately 50 genetic differences in the recent epidemic MPXV genomes. It is concerning that the substitution rate of current MPXV was far more than that previously estimated for orthopoxviruses, and most of the nucleotide substitutions involved conserved features with GA>AA and TC>TT nucleotide replacements [12]. Another study reported similar mutation features in the 2022 MPX cases in the United States [13]. This mutational bias might be associated with the apolipoprotein B mRNA-editing catalytic polypeptide-like 3 (APOBEC3) enzyme, a DNA cytidine deaminase, which inhibits viral replication by editing the viral genome mutations (Figure 1). The excess of 2022 MPXV mutations indicates an accelerated adaptive evolution derived by host APOBEC3. This finding highlights the need of further functional studies to determine whether these mutations contribute to the enhanced transmissibility of the virus or facilitate viral evasion of host immunity.
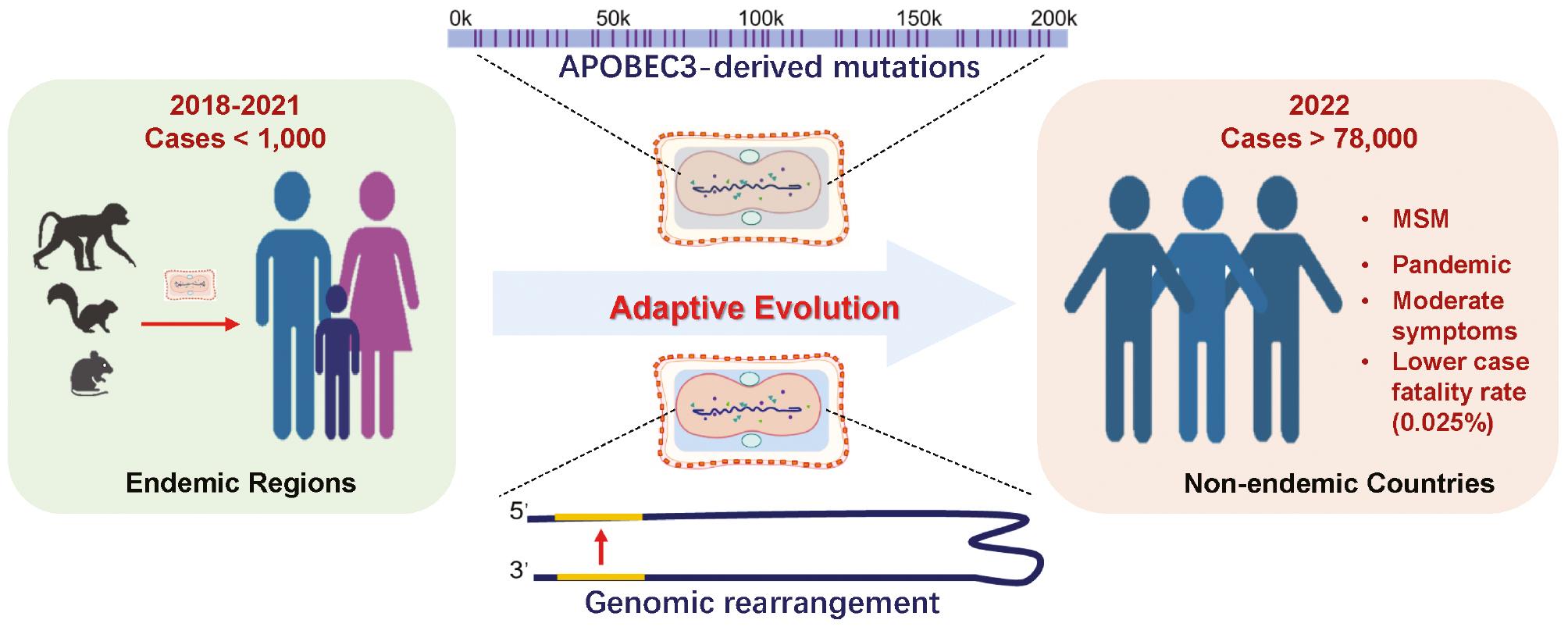
Viral adaptive evolution may be responsible for the new clinical and epidemiologic features of the monkeypox (MPX) outbreak in 2022. Prior to 2022, MPX was a rare zoonosis with limited human-to-human transmission in Central and West Africa. The current MPX outbreak has spread to more than 110 countries with greater than 78,000 confirmed cases. Epidemiologic and phylogenomic analyses indicate that the current MPX outbreak might originate from epidemic regions. Additionally, APOBEC3-derived mutations, as well as viral genomic rearrangement, may lead to viral adaptive evolution which could account for the new clinical-epidemiologic features of the current MPX.
GENOMIC REARRANGEMENTS OF MONKEYPOX VIRUS
In addition to single nucleotide polymorphisms (SNPs), insertions, deletions, and genome rearrangements are commonly detected in the poxvirus genome terminal, which may be associated with altered infectivity and pathogenicity. It has been reported that genome end-region rearrangements have an important role in the virulence and evolution of smallpox virus [14,15]. Genomic rearrangements have also been detected in the current outbreak MPXV. A recent study by Li and colleagues [16] identified a large genomic deletion and rearrangement in MPXV sequences from MSM cases in the United States, where the largest number of cases have been reported. Li et al. [16] found large-scale genomic changes, ranging from 2.3-15kb, involved in several protein coding sequences (CDS) and inverted terminal repeat (ITR) terminal regions. Deletion of the gene encoding a surface glycoprotein (B21L) and zinc finger-like protein (D5R), as well as a truncated ITR, are thought to be involved in immunomodulation, virulence, and the poxvirus host range [14,17]; however, it is too early to determine if these large genomic changes are beneficial, neutral, or harmful to MPXV transmission and pathogenicity. The authors also found a genomic deletion of one sample involved in the target gene of clade II MPXV-specific PCR assays. The large-scale genomic deletion might eventually render the PCR assay ineffective, and PCR assays targeting the terminal regions may be most at risk. Consequently, PCR assays targeting the conserved region or targeting multiple different regions may be necessary to ensure the identification of viruses harboring large deletions. Overall, the emergence of genomic rearrangements highlights the continued need for genomic surveillance of MPXV to study viral evolution during the current epidemic.
In recent decades, refinement of genetic engineering methods based on vaccinia virus have contributed to facilitate the reverse genetic manipulation of poxvirus genomes [18]. Using standard recombination technology, researchers have found that loss of D14L is not the sole virulence factor responsible for the different pathogenicity between MPXV clades 1 and 2 [19]. The observed rapid mutations and large-scale genomic rearrangements in the MPXV genome raise concern that the contemporary circulating strains might be undergoing accelerated evolution with unusual clinical outcomes. Ongoing investigation with reverse genetics will help clarify this issue. More importantly, extensive molecular surveillance and epidemiology investigations are warranted to identify novel mutations that are potentially related to viral transmission, pathogenicity, and escape from available countermeasures.
TREATMENT AND PREVENTION
The two treatments that are currently authorized for MPX (tecovirimat and brincidofovir) inhibit the viral envelop protein, p37, and block viral DNA polymerase, respectively [20]. Several compounds, such as adamantane derivatives, NIOCH-14, PAV-886, mitoxantrone and ribavirin, have been reported to be effective against orthopoxviruses in vitro by blocking p37 formation, viral DNA and protein synthesis, and viral release and entry [21–23]. These compounds enhance the availability and spectrum of the effective antiviral drug against poxviruses; however, the efficacy and safety against the current emerging MPX are largely unknown and require further preliminary and clinical research. As all approved vaccines and antivirals are originally designed to prevent smallpox, whether the vaccines could efficiently prevent the current MPX remains unknown. According to a recent study, vaccination with 2-shot MVA-BN, a third-generation attenuated smallpox vaccine approved for use as a vaccine against MPX, yield relatively low levels of neutralizing antibodies to the epidemic MPXV strain, indicating the need to develop vaccines tailored to prevent current MPXV [24]. Innovative vaccine platforms, like mRNA vaccines, have exhibited excellent protection efficacy and great application prospects during the COVID-19 pandemic, which will facilitate the development of MPX vaccines. To thwart continuation of the current MPX epidemic, it is important to raise awareness and build diagnostic capacity for populations, especially at-risk groups. Additionally, the stigma and discrimination within the MSM community must be eliminated, and equal access to diagnosis, treatment, and vaccines must be provided. Finally, we should initiate global collaborations to evaluate the effectiveness of current treatments, vaccines, and vaccination strategies.

