Abbreviations: CLASP: Edwards PASCAL TrAnScatheter Mitral Valve RePair System Study
Introduction
The Edwards PASCAL Transcatheter Mitral Valve Repair System Study (CLASP) I [1–3] and CLASP IID [4–6] trials assessed the PASCAL system from Edwards Lifesciences for mitral valve repair. CLASP I demonstrated the system’s safety and effectiveness in decreasing mitral regurgitation and ameliorating patient symptoms. CLASP IID further validated the system’s benefits in patients with complex mitral regurgitation who were not ideal candidates for conventional surgery. Together, these trials have provided strong evidence that the PASCAL system is a promising and safe solution for mitral valve repair, particularly for patients at high risk of requiring invasive surgical procedures.
Case Presentation
Our patient, an 84-year-old man with no significant risk factors and no history of smoking has been under medical care since 2012 for mild-to-moderate mitral regurgitation and mild tricuspid regurgitation. His cardiovascular condition worsened in 2014, when he developed permanent bradycardic atrial fibrillation, thus necessitating the implantation of a single-chamber pacemaker (VVI mode) to manage the bradycardia effectively.
In 2015, his condition evolved; an echocardiogram revealed severe mitral regurgitation of mixed etiology, involving both degenerative and functional components. The echocardiogram showed a central regurgitant jet with an area greater than 10 cm2, a vena contracta measuring 8 mm, and a mitral annulus diameter less than 35 mm. The subvalvular apparatus was preserved, but evidence of concentric left ventricular hypertrophy was found, and the ejection fraction had decreased to 0.39, according to Simpson’s method. Given these findings, he underwent mitral valve repair surgery, during which a Sorin Memo 3D (Sorin Biomedica Cardio S.r.L., Saluggia, Italy) 28 mm annuloplasty ring was implanted.
In June 2023, he experienced a domestic accident resulting in a significant hematoma on his right leg, measuring 7 cm in diameter and extending 20 cm in length. This event led to the temporary suspension of his anticoagulation therapy with a non-vitamin K antagonist oral anticoagulant, under careful hematological monitoring to prevent complications. A subsequent CT scan identified a penetrating ulcer in the common iliac artery and an aneurysm of the right internal iliac artery, measuring 4.5 cm in maximum diameter. Because of these vascular findings, his blood pressure was closely monitored to avoid further complications.
A follow-up echocardiogram in July 2023 revealed a decline in global systolic function. Additionally, the mitral valve showed signs of severe regurgitation, characterized by an eccentric jet directed medially. The aortic valve appeared sclerotic with calcified cusps but maintained normal opening function with minimal regurgitation. Given the complexity of our patient’s condition, our heart team decided against surgical intervention for the mitral valve at that time. Instead, he was treated with an endovascular approach using an aorto-bi-iliac stent graft to address the previously identified vascular issues.
By May 2024, his condition had further deteriorated, as evidenced by an increase in the left ventricular end-diastolic dimensions. The mitral valve regurgitation had also worsened and presented as severe with two eccentric jets – one medial and one central – resulting from a dehiscence of the previously implanted annuloplasty ring (Figure 1, and Videos 1 and 2 online) with increased left ventricular dimensions (indexed end-diastolic volume of 76 mL/m2), decreased overall systolic function (Simpson’s ejection fraction of 43%), and left atrial dilation (indexed volume of 76 mL/m2). The transesophageal echocardiogram showed no signs of endocarditic infection, and the dehiscence might have been caused by partial detachment of the pre-implanted ring under the prolonged severe regurgitation. Given these developments, the patient was referred for percutaneous mitral valve repair with the PASCAL Ace (Edwards Lifesciences, Irvine California) system; this minimally invasive option was considered suitable, given his frailty and the risks associated with open-heart surgery.
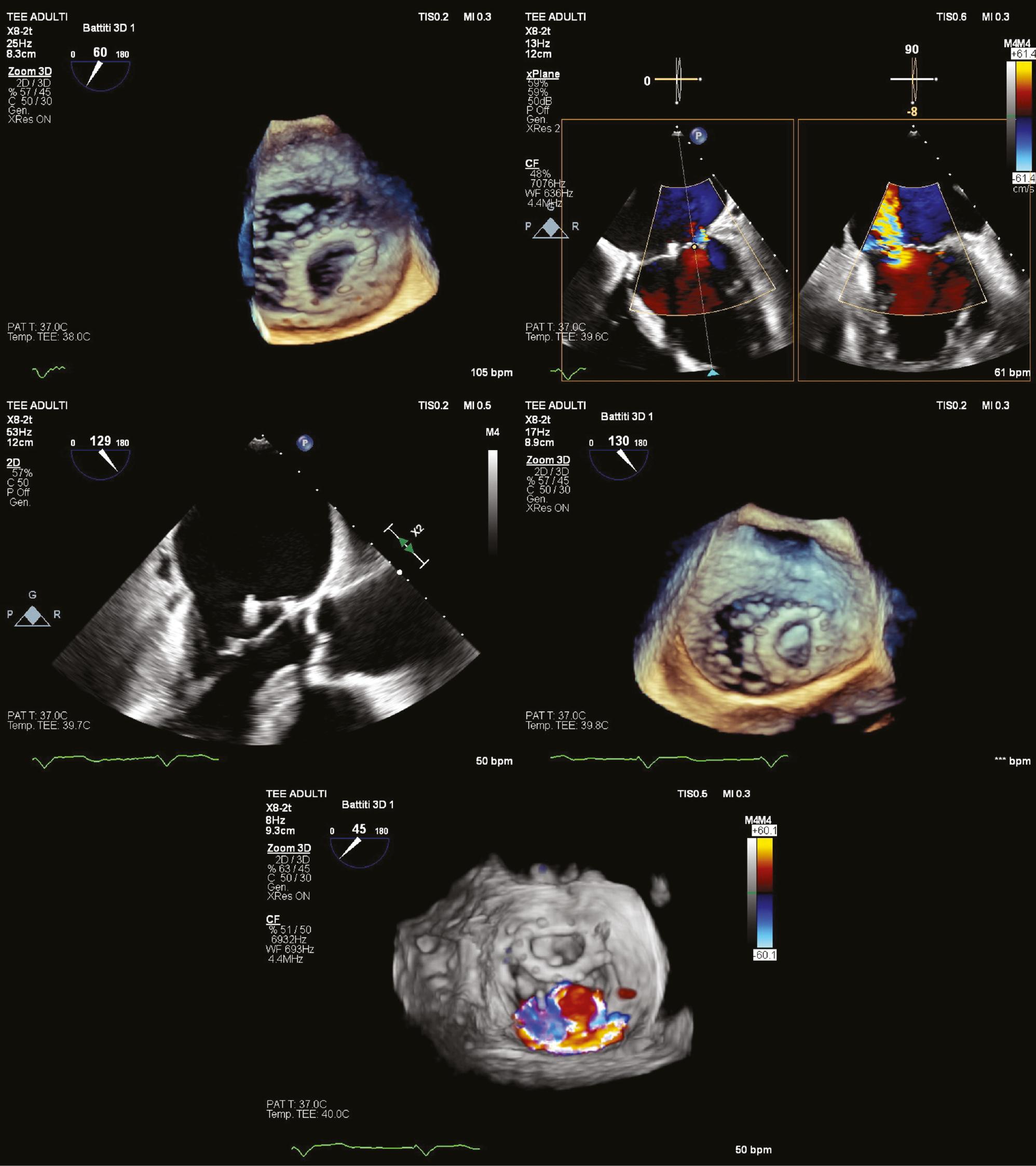
Transesophageal echocardiography (TEE) in a mid-esophageal view, showing, from left to right and top to bottom: 3D surgical view highlighting partial detachment of the prosthetic ring from the mitral plane; evidence of central jet mitral regurgitation; partial ring detachment in 2D; partial ring detachment in 3D; surgical view illustrating the origin and trajectory of the regurgitation jet.
Before the PASCAL system repair, the patient’s therapeutic regimen included insulin, gliflozins, non-vitamin K antagonist oral anticoagulants, diuretics, and sacubitril-valsartan. Dislocation of the annuloplasty ring is a condition for which the standard practice generally involves surgical intervention with valve replacement. However, in our patient, such surgery was not feasible, because of the high operative risk, according to the Society of Thoracic Surgeons Score and other risk factors, including severe left ventricular dysfunction, complex valve disease, and unfavorable mitral valve anatomy, as well as the patient’s diabetes and atrial fibrillation. Despite the limited availability of long-term outcome data on the PASCAL system, the worsening of mitral regurgitation and symptoms, with the patient’s progression to NYHA class III, were decisive factors in the decision to intervene. The challenge lay in successfully navigating the PASCAL system under the dislocated ring.
The PASCAL Ace device was successfully implanted during a 90-minute procedure (Figure 2). The device was introduced via the right femoral vein; subsequently, a transseptal puncture was guided by echocardiography (Videos 3 and 4 online) and fluoroscopy (Video 5 online). The Pascal Ace device was then implanted with anchoring on the A2 and P2 segments of the mitral valve. Despite the dislocated annuloplasty ring, no complications arose during the procedure. After proper placement was confirmed (Video 6 online), the introducer was removed, and the venous access was closed. The procedure was successfully performed without complications and the patient was hospitalized for a total of 6 days and spent only 1 day in the intensive care unit. Post-procedure assessments indicated that his condition had stabilized, and a slight improvement was observed in global systolic function. The residual mitral regurgitation was classified as mild, with the remaining jet located medially (Figure 3). The transvalvular gradient was within normal limits, with a mean gradient of 3.6 mmHg and an effective mitral valve area of 3.5 cm2, split between 1.6 cm2 and 1.9 cm2.
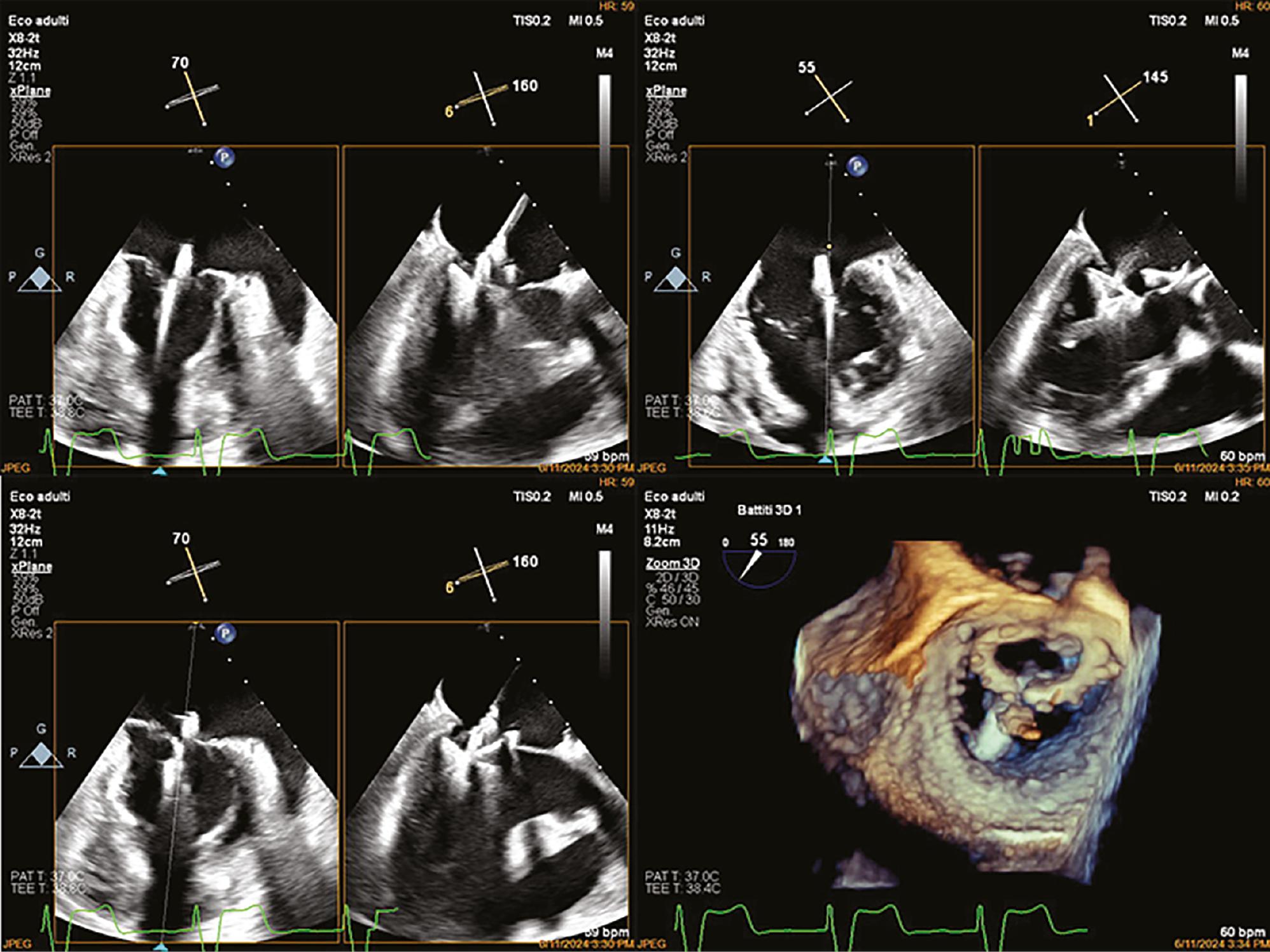
Transesophageal echocardiography (TEE) in a mid-esophageal view, showing, from left to right and top to bottom: the first three images in 2D depict the passage of the Pascal ACE system through the mitral valve, its deployment, correct positioning on A2-P2, and the capture of the mitral leaflets; the remaining image in 3D illustrates the passage of the Pascal ACE system beneath the prosthetic ring.
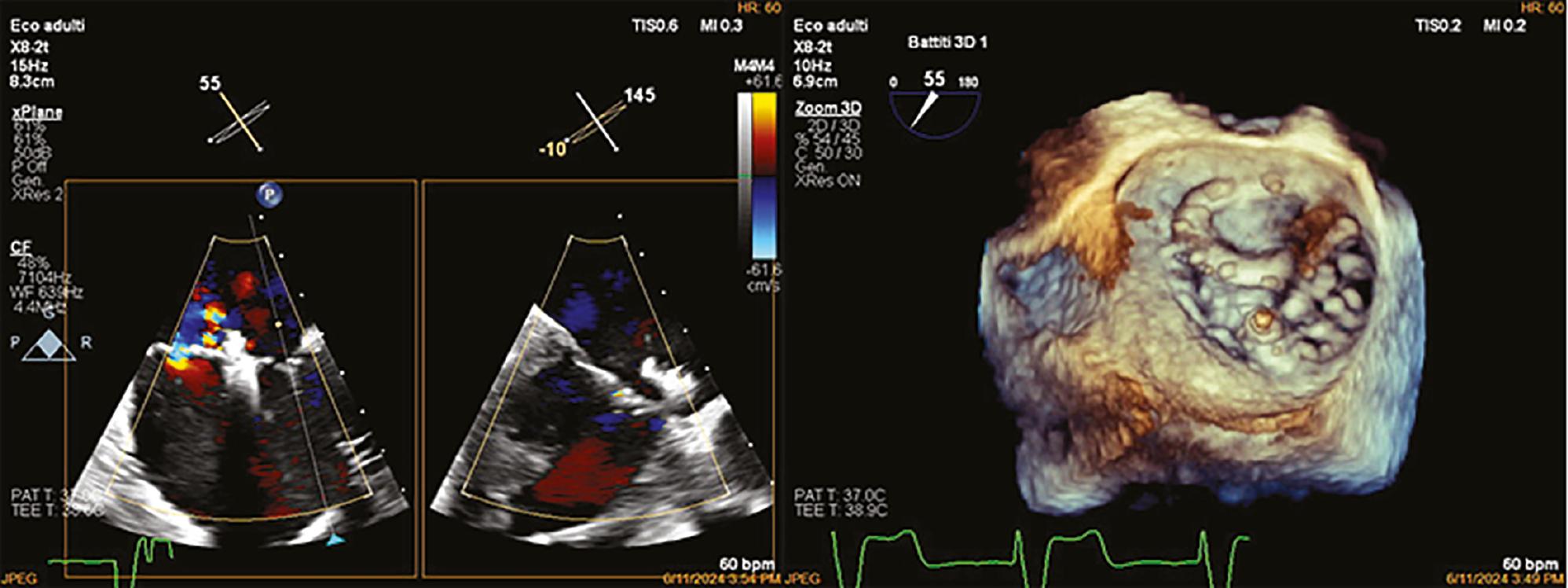
Transesophageal echocardiography (TEE) in a mid-esophageal view showing the correct and effective positioning of the Pascal ACE system in 2D on the left and in 3D on the right.
At the 1-month follow-up, the patient exhibited a notable improvement in cardiac function, and the mitral valve gradient had remained unchanged from the immediate post-procedural assessment. He returned 6 months post-procedure for a follow-up echocardiogram, which showed complete recovery of cardiac function, with Simpson’s ejection fraction >60% (Figure 4), area shortening fraction >0.35, residual mitral regurgitation graded at 1+/4 with a mean gradient of 2 mmHg, aortic regurgitation at 1+/4, and tricuspid regurgitation at 1–2+/4, with a pulmonary artery systolic pressure of 35 mmHg. He reports having resumed a normal lifestyle, including daily use of an assisted bicycle for long distances, without any signs of fatigue or exertional dyspnea. His current treatment regimen includes furosemide, 25 mg; sacubitril/valsartan, 24/26 mg; empagliflozin, 10 mg; allopurinol, 300 mg; edoxaban, 60 mg; nitroglycerin, 5 mg; ursodeoxycholic acid, 150 mg; and digoxin, 0.125 mg. Anticoagulant therapy cannot be discontinued because of the presence of atrial fibrillation.
Discussion
This case illustrates the complexity of managing severe mitral regurgitation in an older patient with multiple comorbidities, particularly when the patient’s condition limits the viability of conventional surgical options. The successful outcome of the percutaneous mitral valve repair with the PASCAL system underscores the potential of minimally invasive procedures in managing high-risk patients.
Both European and American guidelines align regarding the management of patients with annuloplasty ring dehiscence. The European guidelines [7] recommend a customized surgical approach, which might involve the use of specialized annuloplasty devices and consideration of valve repair as part of the surgical strategy. The American guidelines [8] similarly advocate for advanced surgical techniques and specialized devices in managing such cases, emphasizing the need for personalized decision-making based on the severity of the condition and patient-specific factors. A key factor was the role of transesophageal echocardiography, which enabled accurate diagnosis and precise prediction of the intra-procedural scenario; also guided the execution of the procedure and the deployment of the system; and facilitated the assessment of proper positioning and the residual gradient across the mitral valve.
The PASCAL system offers a substantial advancement in the management of severe mitral regurgitation, particularly in patients for whom traditional surgical approaches are deemed too risky. The device’s ability to decrease mitral regurgitation and stabilize cardiac function, as demonstrated in this case, highlights its potential to serve as a viable alternative to more invasive procedures. This case adds to the growing body of evidence from the CLASP trials supporting use of the PASCAL system in managing complex mitral valve disease in high-risk patients.
This case is unique in that it is, to our knowledge, the first instance in Italy and only the second in Europe in which the PASCAL system was used to repair a dislocated annuloplasty ring. The primary challenge was successfully navigating the PASCAL device beneath the dislodged ring without causing entrapment. Because the system was used in an off-label manner, ethical considerations were thoroughly addressed: our heart team carefully evaluated the benefits and drawbacks, given that our patient was 84 years old and highly symptomatic, with severe heart failure. The procedure was complex, and its success was not guaranteed; however, given the patient’s condition, his life expectancy would have been markedly shorter without a successful intervention. After receiving all necessary information, the patient chose to proceed with the procedure.


