Scientific Statement
The 2011 Chinese Society of Cardiology guidelines (2011 CSC guidelines) have provided a key reference for clinical and public health practitioners in preventing cardiovascular disease (CVD) in practice. However, their effects on CVD and its subcategories have not been assessed. This is the first rigorous empirical analysis assessing the extent to which release of the 2011 CSC guidelines decreased incidence, prevalence, mortality, and disability-adjusted life year rates for CVD overall and 13 subcategories. Release of the 2011 CSC guidelines decreased the burden of CVD overall and in several subcategories in China. However, efforts to enhance health education, strengthen primary care, improve the provision of qualified healthcare, and universal healthcare coverage remain urgently necessary to improve cardiovascular health and decrease the CVD burden.
Introduction
Cardiovascular disease (CVD) is the leading cause of premature morbidity and mortality in China, accounting for 43% of deaths [1]. To promote healthy lifestyles and control metabolic risk factors for CVD [2], the Chinese Society of Cardiology (CSC) of the Chinese Medical Association issued the initial Chinese guidelines on CVD prevention in 2011 (2011 CSC guidelines) [3]. The 2011 CSC guidelines emphasize cardiovascular risk assessment based on appropriate 10-year risk evaluation tools for Chinese adults [4–7], and the use of evidence-based interventions (i.e., blood pressure-lowering, smoking cessation, cholesterol-lowering, glucose-lowering, and other pharmaceutical treatments; management of overweight/obesity and kidney injury; and lifestyle and social-psychological changes, such as healthful diets, physical activity, and stress relief) [3].
The CSC guidelines serve as a major reference for clinical and public health practitioners. Quantification of their influence on changes in overall and subtype specific CVD burden (incidence, prevalence, mortality, and disability-adjusted life-years [DALYs]) enables policymakers to optimize the use of health care resources, particularly for primary care. No system exists for monitoring the effectiveness of these clinical guidelines [8]. Few studies have assessed the effectiveness of the CSC guidelines in the context of other initiatives, including the new rural cooperative or changes in basic medical insurance utilization after 2004 [9], and other health promotion programs (e.g., the China Healthy Lifestyle for All in 2007 [10] and the National Plan for the Prevention and Control of Chronic Diseases, 2012–2015, in 2013 [11]). Moreover, changes in population structure, urbanization, living conditions, life expectancy, and air pollution [8, 12] may confound the effects of the CSC guidelines.
We performed Bayesian causal impact analysis [13] by using synthetic controls (i.e., indicators unaffected by the 2011 CSC guidelines) to explicitly model the counterfactual of the CVD burden in the absence of the 2011 CSC guidelines [14], thereby addressing unmeasured bias and confounding. Bayesian causal impact analysis is particularly appropriate when trials are infeasible, and the assumptions of quasi-experimental designs (linear trends for interrupted time series analysis [15], and the assumption of common trends for difference-in-differences designs [16]) are not met [17].
Taking advantage of nationally representative data, we conducted the first empirical study assessing how the 2011 CSC guidelines decreased the incidence, prevalence, mortality, and DALY rates for CVD overall and in 13 subcategories, according to age and sex; brain and central nervous system cancer was used as a negative control unlikely to have been affected by the 2011 CSC guidelines [18].
Methods
Study Design and Data Sources
We conducted a retrospective observational study using Bayesian causal impact analysis [13, 14] to evaluate the effects of the 2011 CSC guidelines versus no guidelines in China for CVD overall and 13 subcategories (i.e., rheumatic heart disease [RHD], ischemic heart disease [IHD], ischemic stroke [IS], intracerebral hemorrhage [ICH], subarachnoid hemorrhage [SAH], hypertensive heart disease [HHD], non-rheumatic valvular heart disease [non-rheumatic VHD], cardiomyopathy and myocarditis, atrial fibrillation and flutter, aortic aneurysm [AA], peripheral artery disease [PAD], endocarditis, and other CVD and circulatory diseases; Supplementary Table 1), according to sex (female, male, and total), and age (25–49, 50–74, and 75+ years).
Data on CVD incidence, prevalence, mortality, and DALY rates by 13 subcategories (age-standardized rate), sex (age-standardized rate), and age group (age group-specific rate) were obtained from the Global Burden of Disease Study (GBD) 2019 [19]. Briefly, GBD 2019 provides systematic, consistent, transparent, and up-to-date metrics of disease burdens from the years 1990 to 2019 for 369 diseases and injuries, in 23 age groups and two sexes, in 204 countries and territories including mainland China, according to a published protocol [20].
We linked the CVD burden estimates to selected indicators from the National Bureau of Statistics of China that might potentially drive the CVD burden but are likely to be independent of the 2011 CSC guidelines [12] (Supplementary Table 2) to generate counterfactual estimates for the CVD burden in the absence of the 2011 CSC guidelines. These indicators were (1) population aging and growth: population size, sex, urban population, crude birth and death rates, population 65 years or older, population density, and life expectancy at birth; (2) availability of medications: number of medical providers, number of health workers, number of medical beds provided, bed occupancy rate for medical providers, and average length of stay for medical providers; (3) affordability of medications: government health expenditure per unit gross domestic product, average wage of employed people in urban non-private settings, disposal income per capita (DIPC), registered unemployment rate in urban areas, cross dependency ratio, and the new rural cooperative medical insurance utilization; and (4) educational attainment (illiterate, primary school, junior secondary school, senior/technical secondary school, and junior college or above).
Outcomes
The primary outcome was the changes in incidence, prevalence, mortality, and DALY rates per 100,000, for CVD overall and 13 subcategories, associated with the 2011 CSC guidelines. Supplementary Table 1 provides definitions and International Statistical Classification of Diseases and Related Health Problem, 10th Revision (ICD-10) codes mapped to CVD overall and 13 subcategories in GBD 2019. The GBD 2019 data were adjusted for varying study methods, case definitions, and study-specific factors, such as data sources and whether first-ever and recurrent cases were included (e.g., IHD, IS, ICH, and SAH), to enable accurate modeling [19].
Statistical Analysis
We estimated changes in the CVD burden caused by the 2011 CSC guidelines after 2011 by using Bayesian causal impact analysis [13, 14], in which the observed CVD burden was compared with the counterfactual estimate of what the burden would have been if the 2011 CSC guidelines had not been issued, as indicated in Supplementary Appendix 1. Briefly, we generated counterfactual estimates for “synthetic controls” [14], in which time-series data for candidate indicators (Supplementary Table 2) were optimally selected and weighted via Bayesian variable selection by fitting the trajectory of CVD burden in China before the 2011 CSC guidelines (pre-introduction period from 1990 to 2010) [13]. The selected indicators were combined into a composite synthetic control, and greater weight was given to indicators that jointly better explained the trajectory of the CVD burden. Because these indicators were not influenced by the 2011 CSC guidelines, the composite synthetic control described the CVD burden during the post-introduction period (2011 to 2019), adjusted for unmeasured bias and confounding.
Using the composite synthetic control, we generated counterfactual estimates for CVD burden in the absence of the 2011 CSC guidelines. We computed the impacts of the 2011 CSC guidelines by using the relative rate decrease (RRR), calculated as 1 minus the median of the ratio between the observed burden and the counterfactual estimate during the post-introduction period. We also calculated the cumulative rates prevented by the 2011 CSC guidelines, by using the sum of the annual absolute difference between the observed burden and the counterfactual estimate during the post-introduction period. A negative value of RRR or cumulative rate prevented indicated an increased burden, whereas a positive value indicated a decreased burden. We calculated 95% uncertainty intervals (UI) by using the 2.5th and 97.5th percentiles of 10,000 Markov chain Monte Carlo (MCMC) samples drawn from the posterior predictive distribution over the counterfactual estimate, given the observed CVD burden, by using the pre-introduction period, [13] and interpreted the 95% UI as the lower and upper boundaries of the estimated guideline-associated impact. For the same MCMC samples, we computed the Bayesian posterior probability (PP or power) of observing any (either increased or decreased) impact of the 2011 CSC guidelines, given the observed CVD burden.
In the main analysis, we considered a 1-year gap between release of the 2011 CSC guidelines and the beginning of the impact (i.e., 2012 to 2019), to allow for potential delayed or gradual effects, as in the first China Salt Substitute Study [21]. Results with different gap years yielded similar conclusions (Supplementary Table 3). The negative control outcome of brain and central nervous system cancer should be unchanged by the 2011 CSC guidelines [18]. Therefore, any effect of the 2011 CSC guidelines on this outcome would indicate potential unadjusted confounding and bias.
We conducted sex- and age -specific analyses. In sensitivity analyses, we removed as many as three indicators with the highest inclusion probability in synthetic controls, based on model 1 (referred to as SC1 without the top one to three indicators). Finally, we triangulated the impact estimates by using model 2, with population size as an offset (for calculating RRR and SC2); model 3, based on model 2, with additional adjustment for a simple linear trend (SC3); model 4, based on model 3, with population size as a covariate (SC4); and model 5, with exclusion of indicators involving population aging and growth (SC5) to generate counterfactual estimates (Supplementary Appendix 1 pp 6–9).
We conducted analyses in R version 4.1.2, using the bsts [22] and CausalImpact [13] packages to construct the synthetic controls and to conduct Bayesian causal impact analysis (Supplementary Appendix 1 pp 13–16), respectively. Sample codes are available on request. We adhered to the guidelines for Accurate and Transparent Health Estimates Reporting: the GATHER statement [23] in reporting the changes associated with the 2011 CSC guidelines in CVD burden, both overall and by subcategory. This analysis of publicly available data did not require ethical approval.
Results
CVD Impact Estimates for the 2011 CSC Guidelines
In China, the CVD incidence rate increased by −1.7% (RRR 95% UI −3.5% to 0.7%; PP 93.7%) in the 9 years after release of the 2011 CSC guidelines, equivalent to −99 (cumulative rate prevented 95% UI −198 to 43) more incident cases per 100,000 (Figure 1). A −1.0% (−3.2% to 0.6%; 92.2%) increase in the prevalence rate was observed, corresponding to −560 (−1 701 to 311) more prevalent cases per 100,000 (Supplementary Table 4), 161 (−152 to 602; 83.8%) prevented deaths, and 1 429 (−4707 to 7621; 70.9%) saved DALYs per 100,000 (Supplementary Table 5). Increased incidence and prevalence with decreased mortality and DALY rates were more evident among men than women. In the 25–49-year age group, the CVD mortality rate declined by 16.0% (−6.6% to 31.8%; 94.0%), i.e., 63 deaths prevented (−21 to 156) and 2376 DALYs saved (−2270 to 7093; 87.1%) per 100,000. Similar impacts were observed in the group 75 years or older, with 1834 deaths prevented (−1735 to 6148; 84.0%) and 22,864 DALYs saved (−15,469 to 68,622; 88.2%) per 100,000, but were not observed in the 50–74-year age group.
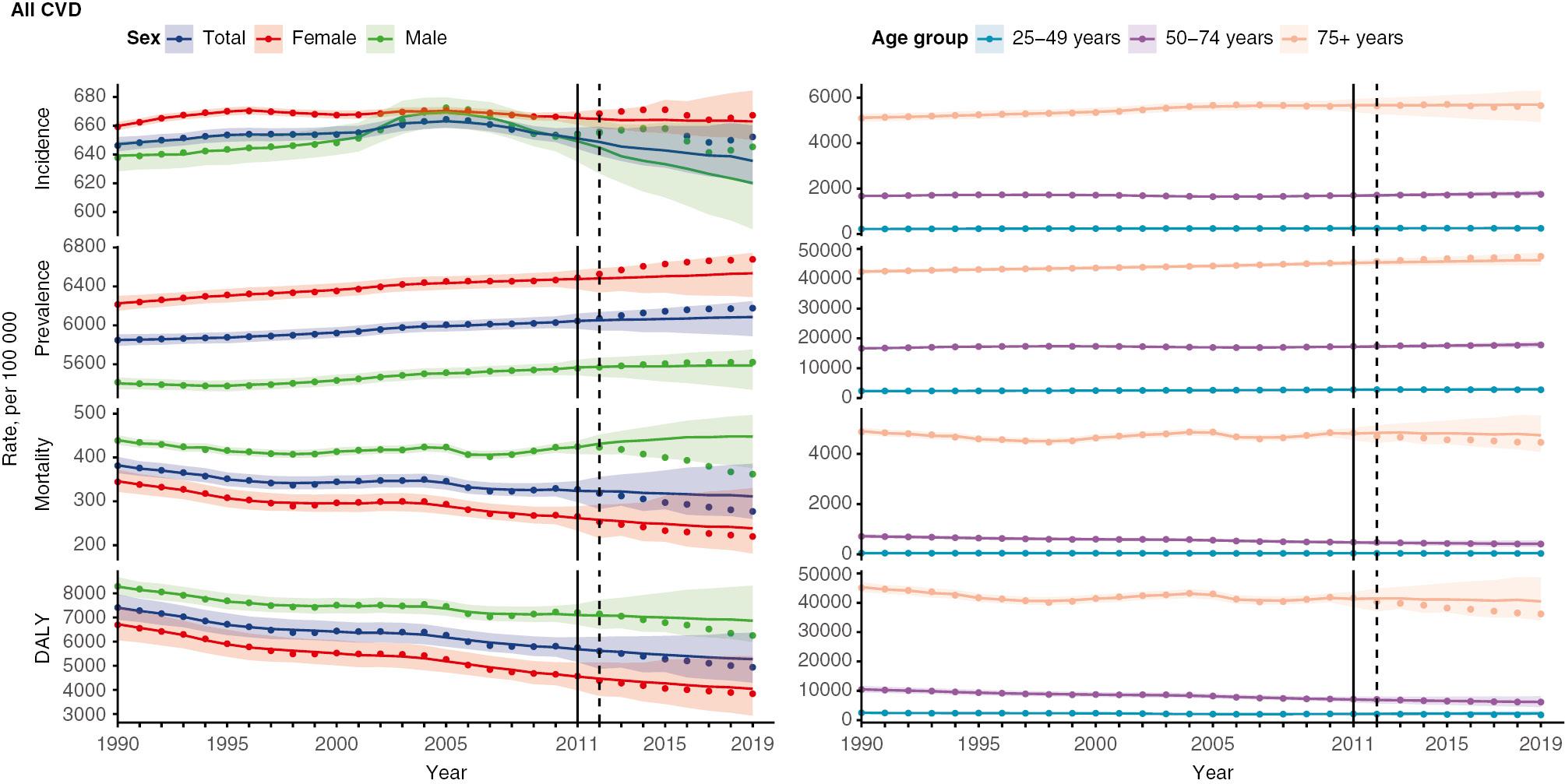
Estimates of Annual Cardiovascular Disease (CVD) Incidence, Prevalence, Mortality, and Disability-Adjusted Life-Year (DALY) Rates per 100,000 in China before and after the Introduction of the 2011 CSC Guidelines, by Sex (Left Panel) and Age Group (Right Panel), with the Composite Synthetic Controls.
Dots represent the observed CVD burden from 1990 to 2019. Solid horizontal lines and shaded areas represent the counterfactual estimates of the CVD burden and the 95% uncertainty intervals in the absence of the 2011 CSC guidelines, on the basis of 1000 Markov chain Monte Carlo samplers. Solid vertical lines indicate the introduction of the 2011 CSC guidelines, and dashed vertical lines indicate the beginning of the evaluation period (i.e., 1-year delay or gradual impact).
CVD Subcategory Impact Estimates of the 2011 CSC Guidelines
First, a desirable pattern with decreasing incidence, mortality, and DALY rates was observed for RHD, IHD, and non-rheumatic VHD. Second, a subdesirable pattern with decreasing mortality and DALY but increasing incidence rates of ICH, IS, cardiomyopathy and myocarditis, and aortic aneurysm was observed. Third, an undesirable pattern with increasing incidence, mortality, and DALY rates was observed for SAH, HHD, atrial fibrillation and flutter, PAD, endocarditis, and other CVD and circulatory diseases (Figure 2). The primary drivers of the increasing burden in the incidence rate were ICH, followed by SAH, and endocarditis, particularly for men and people either 25–49 years of age or 75 years or older. The increases in incidence rates for atrial fibrillation and flutter, PAD, and IS were small (Supplementary Table 4). Moderate-to-mild declines were observed in non-rheumatic VHD and IHD, particularly among women and people 50–74 years of age. These effects on incidence rates translated into modestly increased SAH and IS and decreased non-rheumatic VHD prevalence rates, but had little effect on other CVD subcategories (Supplementary Table 4 and Supplementary Figures 1–13). No effects on the negative control outcome were observed (Supplementary Figure 14).
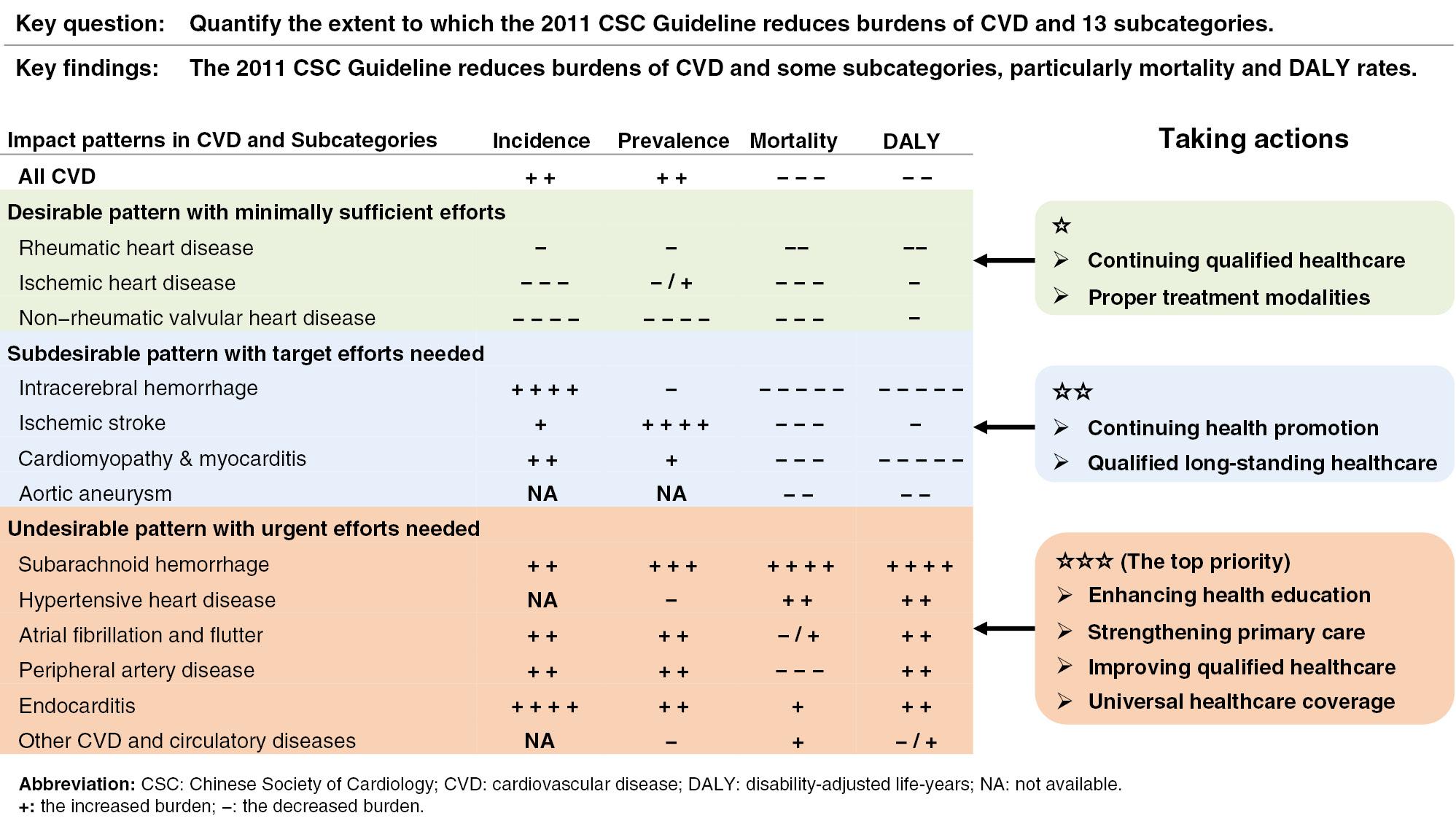
Graphical Illustration of Impact Patterns of the 2011 CSC Guidelines on Cardiovascular Disease (CVD) and 13 Subcategories, in Parallel with Suggested Actions for Decreasing the Burden of CVD and Several Subcategories.
The primary drivers of the decline in CVD mortality after release of the 2011 CSC guidelines were ICH, followed by RHD, cardiomyopathy and myocarditis, non-rheumatic VHD, PAD, IS, IHD, and AA, ranging from a decrease in 8.5% for RHD to 2.4% for AA, particularly among men and people 25–49 years of age (Supplementary Table 5). All subcategories (except PAD) with declining mortality rates also had decreases in DALY rates, ranging from 11.6% for ICH to 1.7% for IS. However, increases in mortality rates were observed for SAH and HHD, with moderate-to-mild effects on endocarditis, other CVD and circulatory disease, and atrial fibrillation and flutter, particularly among women and people 50 years or older. Increased DALY rates were also seen in these CVD subcategories, except for other CVD and circulatory diseases, ranging from −36.2% for SAH to −1.2% for atrial fibrillation and flutter.
Sensitivity and Negative Control Analyses
Figure 3 shows impact estimates for the 2011 CSC guidelines after removal of the three indicators with the highest inclusion probability and use of alternative models with different indicators included, by sex and age group. Quantitatively similar results were obtained (Supplementary Figures 15–27 and Supplementary Tables 6–19). Substantial declines in the incidence, prevalence, mortality, and DALY rates of all CVD were observed after release of the 2011 CSC guidelines, on the basis of alternative models using population size as an offset (i.e., SC2 in Figure 3 and Supplementary Table 6) or adjustment for the linear trend by using population size as an offset (i.e., SC3 in Figure 3 and Supplementary Table 6) or an additional covariate (i.e., SC4 in Figure 3 and Supplementary Table 6). However, these estimates were larger than the observed decline in the CVD burden from 2010 to 2019 in GBD 2019 [1], thus indicating that unmeasured factors distorted the impact of the 2011 CSC guidelines. The primary model (i.e., SC1 in Figure 3) with the indicators included in Supplementary Table 2 sufficiently adjusted for these unmeasured factors and yielded robust impact estimates even after removal of the indicators with the highest inclusion probability (i.e., SC1 without the top one to three indicators in Figure 3) or indicators involving population aging and growth (i.e., SC5 in Figure 3). The null effect of the 2011 CSC guidelines on the negative control outcome validated the estimated impacts (Supplementary Figure 28 and Supplementary Table 20).
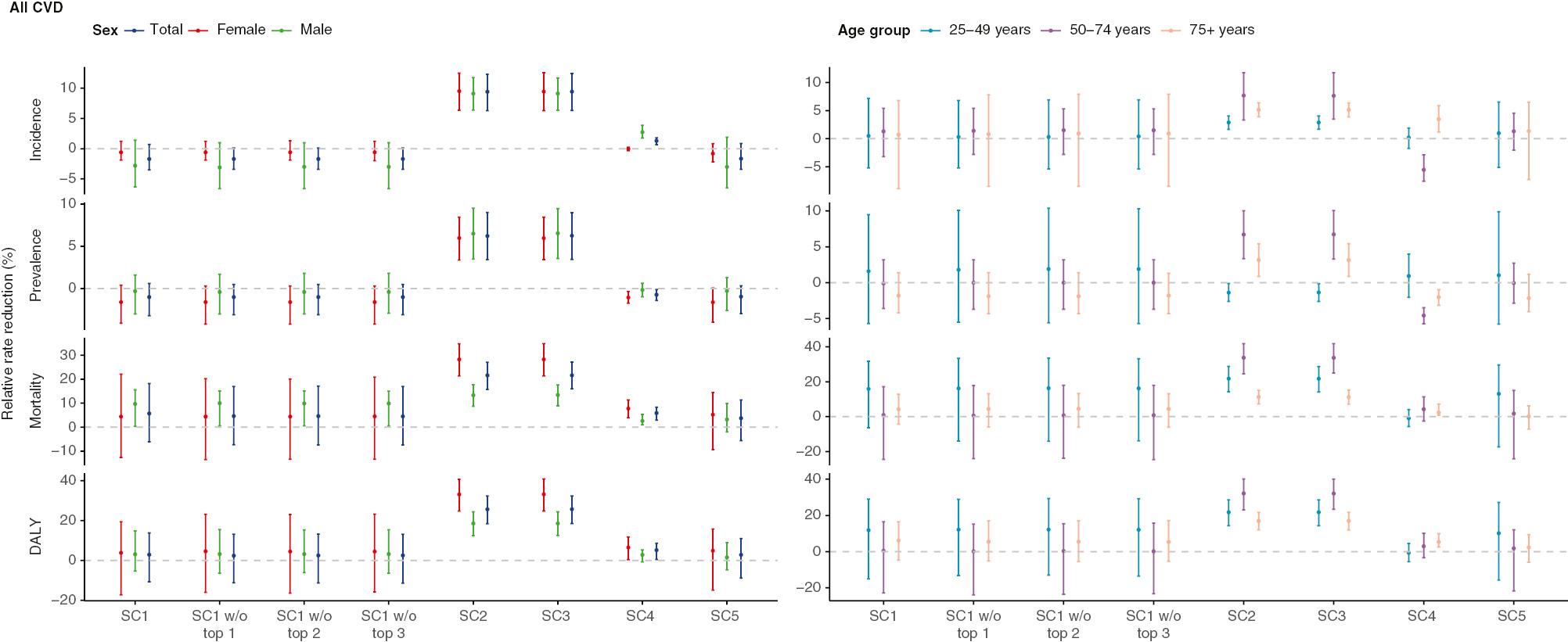
Impact Estimates of the 2011 CSC Guidelines on Cardiovascular Disease (CVD) Incidence, Prevalence, Mortality, and Disability-Adjusted Life-Year (DALY) Rates per 100,000 in China, by Sex (Including Total, Female, and Male) and Age (Including 24–49, 50–74, and 75+ Years), According to Different Models used for Composing the Synthetic Control (SC, Supplementary Appendix 1 pp 8–9).
Briefly, SC1 was derived from model 1, in which all information on indicators was attributed to the transition of CVD epidemiology and current features, but had no influence from the 2011 CSC guidelines. SC1 without (w/o) the top one to three indicators was derived from model 1, with exclusion of the top one to three indicators. SC2 was derived from model 2, with population size considered as an offset. SC3 was derived from model 3, with adjustment for a simple linear trend on the basis of model 2. SC4 was derived from model 4, with adjustment for population size as a covariate, instead of an offset on the basis of model 3. SC5 was derived from model 5, with indicators involving population aging and growth (i.e., population size, urban population, population 65 years or older, population density, birth rate, death rate, and life expectancy at birth) removed from model 1. The dots represent the point estimate of the relative rate decrease as a percentage. The vertical lines represent the 95% uncertainty intervals.
Indicators Contributing to CVD Burden
The three most important indicators (as measured by the inclusion probability) describing all CVD incidence were the number of health workers, population size, and DIPC, which differed from the primarily indicators of CVD prevalence (i.e., urban population, hospital admission rate, and primary school educational attainment) (Figure 4). Most indicators contributing to mortality and DALY rates for CVD were the same, except for the contributions of crude death rates to mortality, and average wage to DALYs.
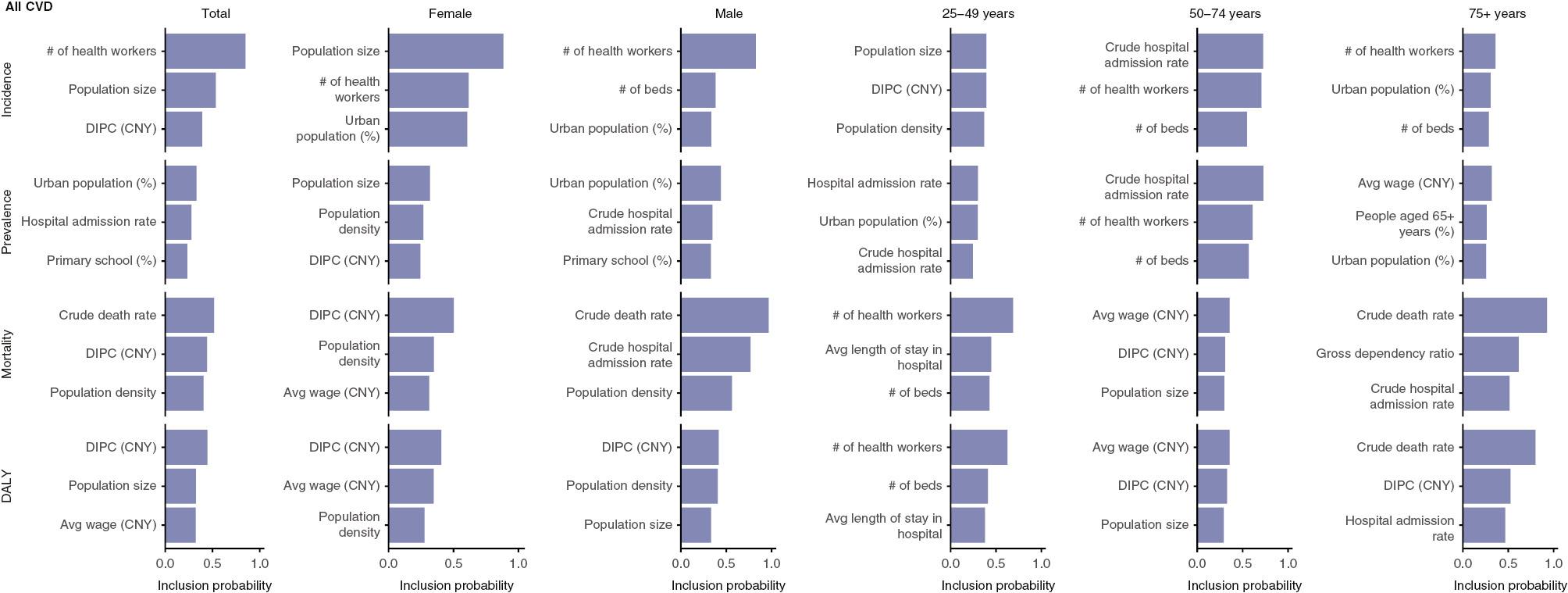
Top Three Selected Indicators with the Highest Inclusion Probability in Composing Synthetic Controls for Cardiovascular Disease Incidence, Prevalence, Mortality, and Disability-Adjusted Life-Year (DALY) Rates per 100,000, by Sex (Total, Female, and Male) and Age (25–49, 50–74, and 74+ Years).
# of health workers: number of health workers per 10,000; population size: population size (year-end, 10,000); DIPC (CNY): disposable income per capita in Chinese Yuan; urban population: proportion of the population living in urban areas in China; hospital admission rate: average number of hospital admissions per 100 outpatients or emergency patients; population density: number of people per square kilometer; Avg wage (CNY): average wage of used people in urban non-private settings in Chinese Yuan; # of beds: number of medical beds provided per 10,000; crude hospital admission rates: number of hospital admission per 10,000; Avg length of stay in hospital: average length of stay for medical providers in days. Details on definitions of the included indicators are presented in Supplementary Table 2.
Most indicators contributing to the CVD burden did not differ by sex. DIPC was more important for women than men, and the crude hospital admission rate was more important for men than women, particularly for prevalence and mortality rates. The DIPC, rather than the number of health workers, was the main contributor to the CVD incidence rate in the 25–49-year age group. Moreover, in contrast to the contributors to CVD incidence and prevalence, the number of health workers, medical beds provided, and average length of stay for medical providers were the leading contributors to mortality and DALY rates. In the group 75 years or older, the gross dependency ratio was the leading contributor to the mortality rate. Supplementary Figures 29–42 show indicators contributing to the burden for 13 subcategories and the negative control outcome after release of the 2011 CSC guidelines.
Discussion
Main Findings
Release of the 2011 CSC guidelines was associated with decreases in mortality and DALYs, but increases in CVD incidence and prevalence rates, with an approximately 1-year lag. Alongside economic development and the launch of multiple national health promotion programs [9–11], the impact of the 2011 CSC guidelines was evident for several CVD subcategories but not others, after adjustment for unmeasured confounding and bias. Furthermore, beyond the 2011 CSC guidelines, several important indicators were found to contribute to CVD and its subcategories, thus supporting prioritization of directions for tailoring appropriate health programs and policies to improve cardiovascular health and decrease the CVD burden in China.
To our knowledge, this is the first rigorous empirical analysis assessing the extent to which clinical guidelines (the 2011 CSC guidelines, in this study) decreased the burden of diseases (CVD overall and 13 subcategories, in this study). Prior studies have extensively discussed the advantages of quasi-experimental designs [15–17] in assessing the impact of a new health policy or initiative when randomized trials are infeasible [15]. However, using the analysis strategies recommended above, we observed a more substantial impact of the 2011 CSC guidelines on the burden of several CVD subcategories than the observed decline from 2010 to 2019 in GBD 2019 [1], thus suggesting that several limitations of quasi-experimental designs merit consideration. For example, the conventional quasi-experimental analyses, on the basis of the stringently linear or common trend assumptions violated in our study, did not fully account for the dynamic changes in population aging and growth, availability, and affordability of medications, or distinguish the impact of the 2011 CSC guidelines from these coinciding changes. Hence, we used Bayesian causal impact analysis [13], an extension of synthetic controls [14], to accurately distinguish the difference in the effects of the 2011 CSC guidelines and the coinciding changes in other factors on the burden of CVD overall and 13 subcategories. In addition, the construction of synthetic controls provided a complementary tool to explore candidate indicators contributing to CVD burden beyond the 2011 CSC guidelines.
Declines in most CVD subcategories occurred after the 2011 CSC guidelines were issued. Rheumatic heart disease, IHD, and non-rheumatic VHD had mild-to-substantial declines in incidence, prevalence, mortality, and DALY rates, thereby suggesting minimally sufficient healthcare. ICH had a substantial increase in incidence, with stable prevalence but substantial declines in mortality and DALY rates, possibly because of the high risk of recurrence in people surviving the first event. Alternatively, release of the 2011 CSC guidelines might have promoted cardiovascular health awareness and hospital visitation, thus resulting in more diagnoses in earlier stages. A similar, suboptimal, impact pattern was also observed for IS, cardiomyopathy and myocarditis, and AA, thus emphasizing the continuing need for health promotion and qualified healthcare, particularly for older people. Subarachnoid hemorrhage, HHD, AF/AFL, PAD, endocarditis, and other CVD and circulatory diseases had a stable or moderate-to-substantial increased burden, thus suggesting that these areas should be major priorities for action and allocation of health resources. These increased burdens might have resulted from more new-onset and non-fatal cardiovascular events, because improved health awareness increased diagnoses after release of the 2011 CSC guidelines [24]. In addition, the updated 2017/2020 CSC guidelines emphasize atherosclerotic cardiovascular disease prevention (including acute coronary syndrome, stable angina, after revascularization, ischemic cardiomyopathy, IS, transient cerebral ischemia, and peripheral arteriosclerosis diseases) [3, 25], rather than heart failure, atrial fibrillation and flutter, and valvular heart diseases.
Identifying factors contributing to CVD burden, in parallel with the CSC guidelines, with target strategies may enhance their effects in the long run. For instance, the 2011 CSC guidelines had a greater impact on Chinese men than women. Unlike basic healthcare affordability (according to the main proxies of DIPC and average wage) in women, cardiovascular health awareness with qualified health care (according to the main proxies of crude hospital admission rate and death rate) is more important in men. Greater impacts of the 2011 CSC guidelines were evident in the 25–49-year age group than in the group 50 years or older, possibly because of birth cohort and period effects. In addition, people 25–49 years of age tended to have higher educational attainment and greater economic prosperity than previous generations, and thus possibly greater health awareness and access to health resources. Non-CVD-specific deaths (e.g., lung cancer) might also have contributed to CVD and subcategory mortality rates, because people, particularly those who are older, can have several comorbidities but die only once [26, 27]. IS and IHD share risk factors; interventions differ in mortality rates, and the prognosis is better for acute IS than IHD [12]. Early CVD deaths prevented by the 2011 CSC guidelines might increase the numbers of people living with IS, recurrent events, or late-onset CVD.
Limitations
Despite comprehensive and robust analyses to assess the impact of release of the 2011 CSC guidelines on the burden of CVD and 13 subcategories, this study has several limitations. First, the limitations inherent to GBD 2019 study [19]. Estimates were obtained by using incidence and death distribution models based on data from censuses and surveillance covering only several counties and districts in remote and less developed provinces of China [28], thus potentially resulting in inconsistent estimates with broad uncertainties, such as RRR for DALY rates of IS, AA, and the negative control outcome. Moreover, the definitions of CVD and 13 subcategories in GBD 2019 might differ from those in the 2011 CSC guidelines, largely because of advances in diagnostic technology (e.g., troponin for acute myocardial infarction) for several subcategories of CVD; thus, our findings should be interpreted carefully.
Second, this study might have overestimated the impact of the 2011 CSC guidelines, because of difficulties in disentangling the effects from other CVD-relevant guidelines introduced around 2011, such as the guidelines for ST-elevation myocardial infarction in 2010 [29], for prevention and treatment of type 2 diabetes in 2013 [30], for prevention and treatment of dyslipidemia in adults in 2007 [31], and for hypertension management in 2010 [32]. No data on the effects of these guidelines are currently available. Third, the indicators used herein might not have fully captured the trajectory of mortality and DALY rates, because of a lack of data on treatment modalities for prevalent cases. For example, people 25–49 years of age have benefitted from strengthened primary healthcare, substantial advances in medical technologies, and rapid economic development since the 1970s [8, 12]; correspondingly, declines in mortality and DALY rates for the negative control outcome occurred after release of the 2011 CSC guidelines. Nevertheless, our results provide valuable information for policymakers to understand the impacts of release of the 2011 CSC guidelines and directions for enhancing impact. Fourth, no region-specific data on the burden of CVD and subcategories are available. Consequently, well-known regional differences [28, 33] could not be explored [34]. Fifth, Bayesian causal impact analysis assumes continuity of the burden of CVD and subcategories and the candidate indicators that existed before release of the 2011 CSC guidelines and continued afterward [13]. The stable burden of CVD and subcategories during 1990–2019 supports this assumption. However, Bayesian causal impact analysis might not entirely rule out unmeasured confounders and bias (e.g., changes in socioeconomic status or air pollution) that might have distorted the observed guideline-associated impact (e.g., PP ≠ 100%) in this study [35]. Nonetheless, qualitatively similar results in sensitivity analyses, along with the larger PP (e.g., PP > 80%), strengthen the credibility of the estimated impacts.
Conclusions
The 2011 CSC guidelines had moderate effects on the burden of CVD overall and in several subcategories in China, particularly mortality and DALY rates in men and people 25–49 years of age. Additional policy efforts to enhance health promotion and strengthen healthcare are needed to improve cardiovascular health and decrease the CVD burden beyond the 2011 CSC guidelines, particularly for SAH, HHD, atrial fibrillation and flutter, PAD, endocarditis, and other CVD and circulatory diseases in China. Further studies are warranted to closely monitor CVD trends and perform rigorous impact assessment of these guidelines, to help prioritize appropriate health programs and policies in China.

