Introduction
Transcatheter device closure of a patent foramen ovale (PFO) is a method commonly used to treat the patient who has experienced a transient ischemic attack (TIA) or cryptogenic stroke because of the PFO. Contrast-enhanced transcranial Doppler (c-TCD) ultrasonography and transesophageal echocardiography (TEE) should be jointly performed to increase the diagnostic accuracy of detecting a PFO [1]. Dextrocardia and situs inversus is a rare medical condition, and no case of a patient with a PFO also experiencing a TIA has previously been reported. We report a patient with mirror-image dextrocardia and situs inversus who experienced a TIA because of the PFO. A Cardi-O-Fix occluder was used to close the PFO with a mirror-reversed rotation of the radiologic views. During the 18-month follow-up, no symptoms of the TIA appeared again.
Case Report
A 26-year-old female patient presented with cough and sputum for 5 days and weakness of her right limb for 10 hours. The patient was hospitalized in the Respiratory Department, and before she arrived at the Inpatient Department, the weakness of her right limb had disappeared. According to her history of past illness, this patient had received a diagnosis of mirror-image dextrocardia and situs inversus. Computed tomography revealed bronchiectasis and pneumonia (Figure 1) but no abnormality in her brain. Echocardiography indicated the possibility of a PFO. A PFO may be the cause of a TIA or even cerebral infarction. Therefore, we considered that the patient had experienced a TIA. TEE was performed, and a PFO with a 1.6 mm left-to-right shunt was found in this patient (Figure 2). c-TCD ultrasonography was also performed. The Valsalva maneuver induced a large number of microembolic signals (Figure 3). After treatment of the bronchiectasis and pneumonia, we had a multidisciplinary team discussion with cardiologists, neurologists, and respiratory physicians. We all agreed that the patient had experienced a TIA, which is due to PFO. We believed that the patient could be at risk of further TIAs because of her job as a flight attendant. We decided to close the PFO with an occluder. The patient was then transferred to the Cardiology Department. Because of the mirror-image dextrocardia and situs inversus, the operation was unusual and difficult for the surgeon. This patient underwent PFO closure through the right common femoral artery approach. Then, the radiologic views underwent reversed rotation (Figure 4A and B). An MPA2 catheter was passed through the atrial septum into the right superior pulmonary vein (Figure 4C). A stiff guide wire was used to replace the MAP2 catheter, and the transport sheath of PFO occluder was placed to the left superior pulmonary vein along the guide wire (Figure 4D, E). The patient then underwent transcatheter closure of the PFO with a Cardi-O-Fix occluder (size 25/25 mm) with use of a 9 F delivery system (Figure 4F–H). The c-TCD ultrasonography findings were negative and the PFO had disappeared postoperatively (Figure 5).
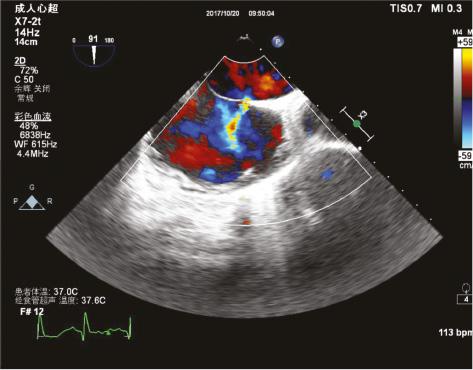
The Patent Foramen Ovale with a 1.6 mm Left-to-Right Shunt Was Found by Transesophageal Echocardiography.
Discussion
Dextrocardia and situs inversus is a rare medical condition that presents as a complete reversal of the internal organs, including the circulatory and gastrointestinal systems. Situs solitus is the most common form (45.4%) of primary fetal dextrocardia, followed by situs ambiguous (36.3%) and situs inversus totalis (18.1%) [2]. The prevalence of situs inversus totalis ranges from 0.3 per 10,000 individuals to 1.4 per 10,000 individuals. Compared with laterality defect cases, most individuals with situs inversus totalis do not have congenital heart disease.
In approximately 30% of young stroke survivors, no clear cause is identified despite a thorough evaluation. A PFO is found on TEE in about half of these patients, compared with approximately 25% of the general population. Some experts recommend PFO closure to prevent future embolic events. Recently, many studies have reported that in patients with a PFO who have had a cryptogenic stroke, the risk of subsequent ischemic stroke was lower among those who underwent PFO closure combined with antiplatelet therapy than among those who received antiplatelet therapy alone [3, 4].
TEE and c-TCD ultrasonography were both performed in this patient to observe the PFO and assess the level of right-to-left shunt. A large number of microembolic signals were found after the Valsalva maneuver. Therefore, we decided to close the PFO of this patient to reduce the risk of TIA.
Percutaneous closure of a PFO in patients with dextrocardia is challenging because it is difficult to choose the best radiologic views and angles. After a thorough review of the literature [5], we determined it was rational to perform the operation by a mirror-reversed rotation of the radiologic views. The previous literature reported that PFO closure in a patient with dextrocardia and situs inversus was performed under the guidance of intracardiac echocardiography [6], while in our case the operation was performed under the guidance of digital subtraction angiography. In addition, compared with the previous literature, the patient was followed up for 18 months in our case.
Follow-up
The patient continued with medical therapy with aspirin at 100 mg per day and clopidogrel at 75 mg per day for 6 months after the closure of the PFO. Repeated TEE found no sign of left-to-right shunt, and the position of the occluder was stable. c-TCD ultrasonography also found no microembolic signals both at rest and after the Valsalva maneuver 10 months after the operation. During the 18-month follow-up period, our patient felt better, with no dizziness, headaches, or any other symptoms of a TIA, and at the end of the follow-up period she had been pregnant for 2 months. In addition, we advised the patient to avoid colds during the pregnancy, to avoid X-rays, to take folic acid supplements, and to receive regular prenatal care.
Conclusion
This is the first report of percutaneous closure of a PFO in a patient with dextrocardia and situs inversus under the guidance of digital subtraction angiography. A Cardi-O-Fix occluder (size 25/25 mm) was used to close the PFO with a mirror-reversed rotation of the radiologic views. No left-to-right shunt was found on repeated TEE, and no microembolic signals were found on repeated c-TCD ultrasonography 10 months after the operation. The results at the 18-month follow-up are satisfactory, the patient has exhibited no further symptoms of the TIA, and the position of the occluder is stable.





